How the No Surprises Act IDR Is Driving Employer Costs

When “No Surprises” Means Higher Costs: How the No Surprises Act’s IDR Process Is Increasing Employer Spend.
Key Takeaways
-
Independent Dispute Resolution (IDR) is creating cost burden in both awards and operations. Employers face higher effective payment levels (often multiples of benchmark ratees) plus significant fees and growing operational costs as carriers scale IDR response capabilities.
-
A few high volume players are driving outsized impact. For certain providers and third party firms, IDR is a revenue strategy, creating localized cost and volatility hotspots.
-
Employers must treat IDR as a strategic cost issue. Plan sponsors should demand clear IDR reporting, shape carrier negotiation and arbitration strategies, and factor IDR performance into carrier and network decisions.
The federal No Surprises Act (NSA) has largely delivered on its promise of shielding patients from most surprise medical bills. But four years into implementation, attention is focused on an unintended side effect of the law’s Independent Dispute Resolution (IDR) process: rising costs for employers and health plans.
When the NSA originally passed, it was widely expected to lower costs on the theory that eliminating balance billing would reduce providers’ leverage, drive more providers in‑network and pull payments closer to median contracted rates. However, early experience shows the opposite dynamic emerging.
Intended as a limited backstop when payers and providers couldn’t agree on a reasonable out of network payment, IDR has evolved into a high volume, high stakes arena with real financial consequences. IDR case volumes are now over 100 times higher than initial federal projections, providers are prevailing in the vast majority of disputes, often at levels well above benchmark payments, and insurers are beginning to quantify IDR as a measurable driver of medical trend.
IDR as a Business Model
Market behavior suggests that for a subset of providers, IDR is no longer a last resort—it is a business strategy, and that strategy is helping to create sharp geographic differences in dispute volumes. Arbitration activity is being driven disproportionately by “frequent flyer” organizations that file disputes at scale, often through specialized third parties. HaloMD is a leading example: as a third party firm that manages the IDR process for thousands of providers, it filed more disputes than any other initiating party in the first half of 2025, accounting for nearly 20% of all federal IDR submissions with more than 230,000 total disputes filed.
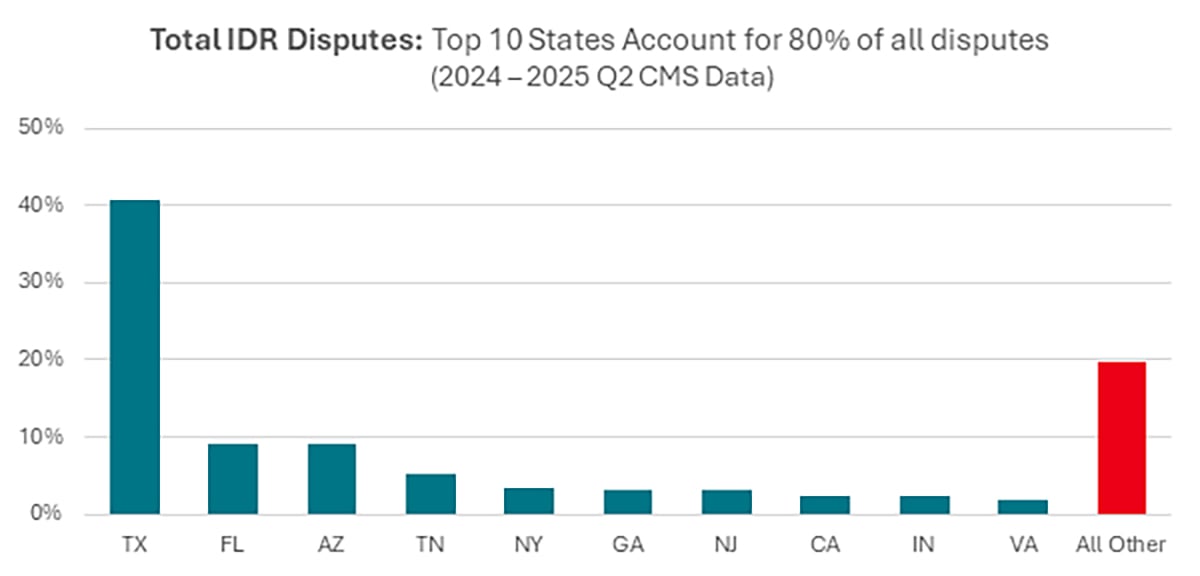
The outsized role of Texas based HaloMD and similar entities helps explain why IDR volume is heavily concentrated in certain states rather than evenly distributed across the country. Texas, in particular, has emerged as a national outlier, accounting for nearly 40% of all federal IDR disputes in the first half of 2025. Other high volume states (e.g. Arizona, Florida) show a similar pattern: a relatively small set of large provider organizations and their IDR intermediaries account for a disproportionate share of filings.
Payers report that in these hotspot markets, groups working with high volume IDR vendors are systematically routing a large share of claims into arbitration, treating IDR as a routine revenue lever rather than an exception pathway. For national employers, the result is that NSA related IDR is not just a broad national phenomenon but a localized risk: costs and volatility are concentrated in a handful of states and metro areas where players like HaloMD and their affiliated providers are most active.
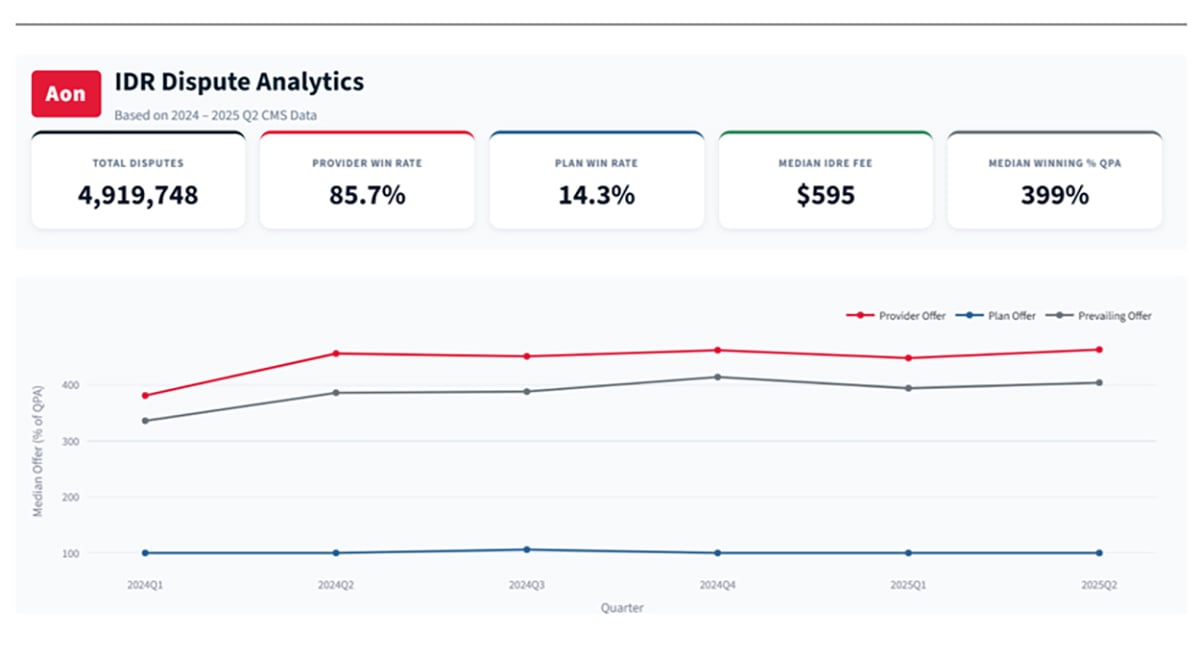
A Growing Cost Burden
Public federal reporting over the past several cycles shows consistent patterns. The number of disputes initiated continues to grow with IDR volumes increasing nearly 40% from the first half of 2024 to the first half of 2025. Additionally, providers’ offers are selected in the vast majority of disputes - approximately 85% of the time - with median IDR awards that are several multiples of the Qualifying Payment Amount (QPA) at roughly four times the benchmark.
The IDR fees alone are staggering. These fees include both an administrative fee as well as a fee paid to the IDR entity adjudicating each dispute. Total federal administrative fees and IDR entity compensation exceeded $800M in the first half of 2025 - but these fees are only a small piece of the equation:
- The disproportionately high results in favor of providers have some carriers voicing that IDR is adding visible basis points to trend. In a February earnings call, major insurer Centene, reported the No Surprises Act’s IDR process as a visible contributor to their 1% increase in medical loss ratio.
- Beyond dispute fees, the process is generating significant structural administrative overhead to stand up IDR operations, with carriers – particularly those that operate in hard hit states – reporting that the overwhelming volume of cases is requiring them to expand teams to support the caseload.
For large employers, these dynamics are now embedded in the health cost equation. Even if the IDR process is largely invisible to members and HR teams, it is driving real dollars at both the claim level and the administrative level.
What Employers Should Do Now
For most employers, the mechanics of managing individual IDR cases resides with their carrier or TPA partner. While operationally convenient, this can be strategically incomplete. The scale and direction of IDR trends mean that plan sponsors need to play an active role in monitoring their costs and asking targeted strategic and governance questions:
-
1. Elevate IDR from Compliance Topic to Strategic Risk
Employers should push for clear visibility into IDR performance and financial impact, including:
- Volumes and trends in IDR filings by service category, provider type, and geography,
- Default rates, Win/loss rates, and median awards relative to the QPA,
- Identification of top provider groups driving disputes, particularly in IDR dense markets like Texas, and
- Quantification of medical and administrative cost impacts attributable to IDR.
-
2. Define Your Plan’s Strategy for IDR
Armed with data, sponsors can more effectively challenge, validate, or refine their carriers’ negotiation and arbitration strategies. Employers should provide direction on questions such as:
- How aggressive or conservative should carrier offers be in categories with high dispute rates and unfavorable arbitration trends?
- Under what circumstances should plans lean toward higher negotiated payments before a dispute is filed to avoid potentially worse outcomes through IDR?
- How should IDR performance (e.g. win rates, award levels, and dispute volumes, etc.) factor into carrier selection, performance guarantees, and network design decisions?
- What expectations should carriers meet around IDR management (negotiation philosophy, escalation thresholds, and reporting transparency and cadence)?
With clear direction, HR, finance, and legal stakeholders can ensure carriers manage IDR related decisions in a way that reflects the organization’s overall objectives.
The Bottom Line
The No Surprises Act has significantly reduced catastrophic surprise bills for employees and their families—a major win for member financial protection. But the statute’s IDR mechanism is not, on its own, a cost reduction tool for employers.
Instead, emerging evidence points to:
- Higher effective payment levels in key niches, with arbitration decisions skewing toward provider offers at multiples of the QPA;
- Concentrated financial risk driven by a relatively small set of high IDR provider groups and geographies, including outsized dispute volumes in specific geographies; and
- New structural administrative complexity and cost as carriers and TPAs build and run IDR operations at scale.
Employers that take a proactive, data driven stance will be better equipped to manage costs and avoid unwelcome surprises on their benefit plans.
Sources:
Federal IDR Supplemental Tables and Public Use Files (2023-2025),
Centene Q4 2025 Earnings Call Transcript,
How a Texas couple is getting rich off out-of-network medical bills,
Congress must fix the No Surprises Act before it bankrupts patients and employers,
Fact Sheet: Clearing the Independent Dispute Resolution Backlog,
The Implications of the No Surprises Act on Contract Dynamics, Negotiations, and Finances
General Disclaimer
This document is not intended to address any specific situation or to provide legal, regulatory, financial, or other advice. While care has been taken in the production of this document, Aon does not warrant, represent or guarantee the accuracy, adequacy, completeness or fitness for any purpose of the document or any part of it and can accept no liability for any loss incurred in any way by any person who may rely on it. Any recipient shall be responsible for the use to which it puts this document. This document has been compiled using information available to us up to its date of publication and is subject to any qualifications made in the document.
Terms of Use
The contents herein may not be reproduced, reused, reprinted or redistributed without the expressed written consent of Aon, unless otherwise authorized by Aon. To use information contained herein, please write to our team.
Aon's Better Being Podcast
Our Better Being podcast series, hosted by Aon Chief Wellbeing Officer Rachel Fellowes, explores wellbeing strategies and resilience. This season we cover human sustainability, kindness in the workplace, how to measure wellbeing, managing grief and more.
Aon Insights Series Asia
Expert Views on Today's Risk Capital and Human Capital Issues
Aon Insights Series Pacific
Expert Views on Today's Risk Capital and Human Capital Issues
Aon Insights Series UK
Expert Views on Today's Risk Capital and Human Capital Issues
Client Trends 2025
Better Decisions Across Interconnected Risk and People Issues.
Construction and Infrastructure
The construction industry is under pressure from interconnected risks and notable macroeconomic developments. Learn how your organization can benefit from construction insurance and risk management.
Cyber Resilience
Our Cyber Resilience collection gives you access to Aon’s latest insights on the evolving landscape of cyber threats and risk mitigation measures. Reach out to our experts to discuss how to make the right decisions to strengthen your organization’s cyber resilience.
Employee Wellbeing
Our Employee Wellbeing collection gives you access to the latest insights from Aon's human capital team. You can also reach out to the team at any time for assistance with your employee wellbeing needs.
Environmental, Social and Governance Insights
Explore Aon's latest environmental social and governance (ESG) insights.
Q4 2023 Global Insurance Market Insights
Our Global Insurance Market Insights highlight insurance market trends across pricing, capacity, underwriting, limits, deductibles and coverages.
Global Risk Management Survey
Better Decisions Across Interconnected Risk and People Issues.
Regional Results
How do the top risks on business leaders’ minds differ by region and how can these risks be mitigated? Explore the regional results to learn more.
Impact Report 2025
Explore Aon's corporate sustainability impact and strategy.
Top 10 Global Risks
Trade, technology, weather and workforce stability are the central forces in today’s risk landscape.
Industry Insights
These industry-specific articles explore the top risks, their underlying drivers and the actions leaders are taking to build resilience.
Human Capital Analytics
Our Human Capital Analytics collection gives you access to the latest insights from Aon's human capital team. Contact us to learn how Aon’s analytics capabilities helps organizations make better workforce decisions.
Human Capital Quarterly Insights Briefs
Read our collection of human capital articles that explore in depth hot topics for HR and risk professionals, including using data and analytics to measure total rewards programs, how HR and finance can better partner and the impact AI will have on the workforce.
Insights for HR
Explore our hand-picked insights for human resources professionals.
Workforce
Our Workforce Collection provides access to the latest insights from Aon’s Human Capital team on topics ranging from health and benefits, retirement and talent practices. You can reach out to our team at any time to learn how we can help address emerging workforce challenges.
Mergers and Acquisitions
Our Mergers and Acquisitions (M&A) collection gives you access to the latest insights from Aon's thought leaders to help dealmakers make better decisions. Explore our latest insights and reach out to the team at any time for assistance with transaction challenges and opportunities.
Natural Resources and Energy Transition
The challenges in adopting renewable energy are changing with technological advancements, increasing market competition and numerous financial support mechanisms. Learn how your organization can benefit from our renewables solutions.
Navigating Volatility
How do businesses navigate their way through new forms of volatility and make decisions that protect and grow their organizations?
Parametric Insurance
Our Parametric Insurance Collection provides ways your organization can benefit from this simple, straightforward and fast-paying risk transfer solution. Reach out to learn how we can help you make better decisions to manage your catastrophe exposures and near-term volatility.
Pay Transparency and Equity
Our Pay Transparency and Equity collection gives you access to the latest insights from Aon's human capital team on topics ranging from pay equity to diversity, equity and inclusion. Contact us to learn how we can help your organization address these issues.
Property Risk Management
Forecasters are predicting an extremely active 2024 Atlantic hurricane season. Take measures to build resilience to mitigate risk for hurricane-prone properties.
Technology
Our Technology Collection provides access to the latest insights from Aon's thought leaders on navigating the evolving risks and opportunities of technology. Reach out to the team to learn how we can help you use technology to make better decisions for the future.
Trade
Our Trade Collection gives you access to the latest insights from Aon's thought leaders on navigating the evolving risks and opportunities for international business. Reach out to our team to understand how to make better decisions around macro trends and why they matter to businesses.
Transaction Solutions Global Claims Study
Better Decisions Across Interconnected Risk and People Issues.
Weather
With a changing climate, organizations in all sectors will need to protect their people and physical assets, reduce their carbon footprint, and invest in new solutions to thrive. Our Weather Collection provides you with critical insights to be prepared.
Workforce Resilience
Our Workforce Resilience collection gives you access to the latest insights from Aon's Human Capital team. You can reach out to the team at any time for questions about how we can assess gaps and help build a more resilience workforce.
More Like This
-

Article 13 mins
AI Risk 2026: What Business Leaders Need to Know
The accelerating role of artificial intelligence in organizational decision making in 2026 is redefining exposure — from fraud to operational resilience. Leaders must strengthen controls, build clear accountability, and ensure their risk and insurance programs keep pace with AI‑driven threats.
-

Article 5 mins
A New Pension Roadmap for Plan Sponsors
Defined benefit (DB) pension plan management has entered a new era. Learn more about the different tools and approaches plan sponsors need to meet their long-term goals.
-

Article 11 mins
Bridging the Gap: Solutions for Managing Construction-to-Operation Transition Risk
Construction-to-operation transitions are rarely seamless. Without clear responsibilities, precise handover definitions and aligned insurance structures, critical risks can fall through the cracks — but early coordination can help.